Report
of the Faculty Welfare Committee on HealthChoice
In January, 2004, the Faculty Welfare
Committee submitted a brief questionnaire on HealthChoice to the faculty,
staff, and retirees. At that time, the
university had been insured under HealthChoice and Pacificare for barely six
months, and it was already in the process of soliciting bids from private
insurance companies to determine whether there are viable alternatives to the
health care plans offered by the State of
We should express several caveats at the
outset of our report. First, those who
responded to our questionnaire constitute a small fraction of the total number
of faculty, staff, and retirees at the
Summary
The Committee’s major findings include the following:
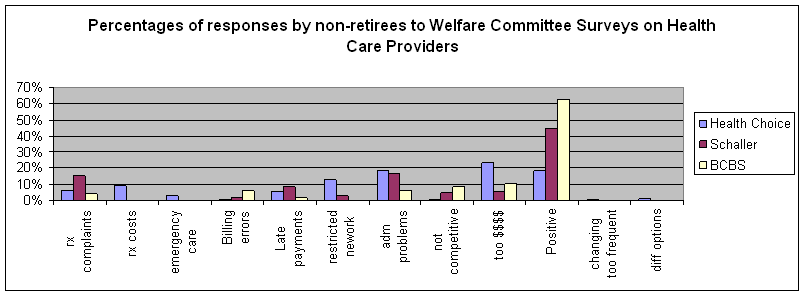
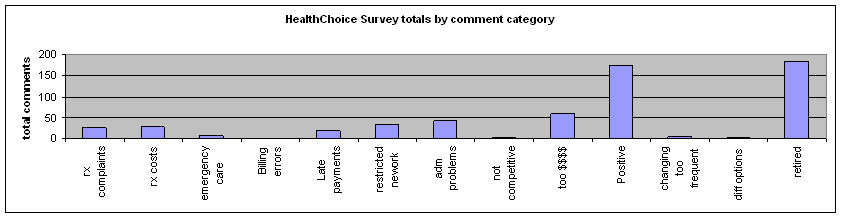
The following categories correspond to those used for a 2002 survey of the Schaller-Anderson and Blue Cross-Blue Shield health plans then used by the university. The accompanying bar graphs compare responses from the two surveys in each category.
Positive Comments:
University employees submitted many positive comments about HealthChoice. Some respondents applaud the fact that Health Choice has no lifetime benefits cap, and they appreciate the fact that a PPO, as opposed to an HMO, allows them to see specialists without having to secure a referral from their primary care physician. Others mentioned that HealthChoice pays for some treatments and preventive screening that BC/BS does not. For example, a psychologist on the faculty praised HealthChoice for not being “too limiting in terms of which psychiatric diagnoses they’ll reimburse for,” including Attention Deficit Disorder. Blue Cross/ Blue Shield is, to use her word, “exclusionary.” Another employee found HealthChoice’s “service to be exceptional” and yet another observed that “[t]heir case workers are wonderful to work with.”
Support for HealthChoice is even more
notable among retirees. Retirees fall
into two groups: those 65 and older who
use HealthChoice as a supplement to Medicare, and those under 65 who use
HealthChoice as their primary, if not exclusive, insurance. In the former case, Medicare pays about 80%
of medical costs and HealthChoice the remainder. These retirees generally have a very positive
view of HealthChoice, and few want the university to change plans. Their complaints are relatively minor, and most
relate to prescription drug coverage. A considerable
number of the faculty and staff have a suspicious if not hostile view of
HealthChoice, but the retirees indicated that claims were paid promptly, few
claims were rejected, and HealthChoice provided good service. Indeed, some think that HealthChoice has been
easier to work with than either Blue Cross/Blue Shield or Schaller-Anderson. Even those who sought out-of-state or out-of-network
physicians and hospitals had few complaints.
For example, one woman had breast cancer surgery at M. D. Anderson in
Too Expensive:
Current faculty and staff dislike being asked to pay more for a plan that has higher deductibles. One described the deductibles as “so high that I barely have any benefit of coverage.” Some can’t afford to insure dependents under the plan, and others fear that faculty recruitment and retention will suffer from the sharp increase in premiums for dependent coverage. Since most retirees use Medicare as their main provider and the university pays the cost of each retiree, there are few complaints about the plan being too expensive. Retirees under 65 are in the same situation as active employees. Indeed, several retirees who expressed concern about the cost of prescription drugs wanted the option to purchase a more expensive plan with lower deductibles and co-pays.
Prescription Benefits
The most common complaints concerning prescription benefits relate to the cost of medicines and the restriction of coverage to a list of approved drugs. Of the 54 cost or coverage complaints, about half relate to cost and the other half to coverage. Few respondents mentioned the “prior approval” merry-go-round, but there were complaints that even after a physician recommended a particular drug, HealthChoice refused to approve it. One respondent said that he had switched to Pacificare because of the better prescription coverage. (On the other hand, at least one respondent said that he was able to obtain a waiver.) Limitations on time between refills were also mentioned by a few respondents. One recounted that his pharmacist had to break six pills from a blister pack of nine pills because of such requirements. Nevertheless, problems with prescription coverage are fairly limited. Of more than 300 responses, only 27 complaints related to this coverage. Nevertheless, to those whose doctor writes a prescription for a medicine not on the approved list, the “hassle factor” appears to be significant. Among retirees, the cost of prescriptions is the principal concern.
Late Payments
Responses in this category are easily summarized by the initials STP—Slow to Pay. Of 19 total responses, all but four fit into this category. With so few out of the 300+ replies indicating this difficulty, the problem does not appear to be pervasive. Nevertheless, since respondents were implicitly comparing their recent experience with that of earlier providers, this is an issue that bears attention. Perhaps HealthChoice has statistics to indicate what the turnaround time is and how their performance compares with national averages.
Two respondents mentioned delays that resulted from their failure to fill out a form HealthChoice evidently requires stipulating that a child dependent is not covered by other health insurance. This form must be filed by the insured parent before the provider will honor coverage for his or her children. In these cases, there appeared to be a lack of communication between provider and participant about the need to fill out the form. Significant delays resulted. This problem could easily be solved.
To the extent that retirees responded in this complaint category, the response was nearly a unanimous complaint about the timeliness of payments.
Billing Errors
There was only one complaint about billing. To quote the respondent: “Twice I have received bills for additional fees that were not charged to me at the time of service. So it’s very unclear how much services are going to cost.”
Emergency Care
Most emergency care
responses focus on the emergency room at
Not Competitive with Outside Options
There was only one response in this category. It argued for the need to look for providers that might provide more competitive rates.
Coverage is Too Costly
Few faculty or staff were prepared for the changes that resulted from the movement to a new provider. HealthChoice appears to many former members of Blue Cross and Schaller-Anderson as less generous and more restrictive. Most complaints related to cost of coverage. Many individuals felt that the cost of deductibles and co-pays limited the value and usefulness of HealthChoice. Others complained that increasing premiums and deductibles put an undue strain on families with multiple dependents. Prescription costs were also seen as burdensome. Some individuals claimed that they were forced to pay for routine tests covered by previous providers that they assumed HealthChoice would also cover. In general, the responses in this category were pleas for relief.
Administrative Problems
Many problems related to the administration of Health Choice grow out of the paperwork required to process claims. Some respondents complained of submitting multiple claims because the original was “lost” or went to the wrong office. In other cases, claimants were told forms had been mailed to them when no such forms had been sent. There are also a few complaints about the way participants were treated on the phone when making inquiries about claims. And several respondents claimed they had not received an insurance card after over six months of membership in the plan. These may be isolated cases, but they create considerable ill-will among “neglected” plan members.
Delayed Explanation of Benefits:
This is not a major issue with retirees. HealthChoice pays what Medicare will not, and few retirees have any complaints. However, some current employees and staff claim that they expected a particular test or service to be covered and later found that it was not. HealthChoice picks up some “preventive” costs routinely, such as flu shots, but applies the annual deductible to others, suggesting that many “misunderstandings” arise from a lack of knowledge of how the plan operates. Nevertheless, some respondents think that HealthChoice gives them the “runaround,” either by requiring them to submit paperwork repeatedly, or by refusing to accept a physician’s judgment or recommendation.
Restricted Network/Out of Network:
Even making allowances for the anxiety
incidental to the change-over from Schaller-Anderson and BC/BS to HealthChoice,
the concerns of faculty and staff with restricted network and out-of-network
care deserve careful consideration, particularly the plan’s coverage outside
Recommendations
The Faculty Welfare Committee:
Donald J. Pisani, Chair (History Department)
Robert Dauffenbach (Center for Economic & Management Resources)
Pat L. Weaver-Meyers (Bizzell Library)
G. Lee
Willinger (

